Care Coordination
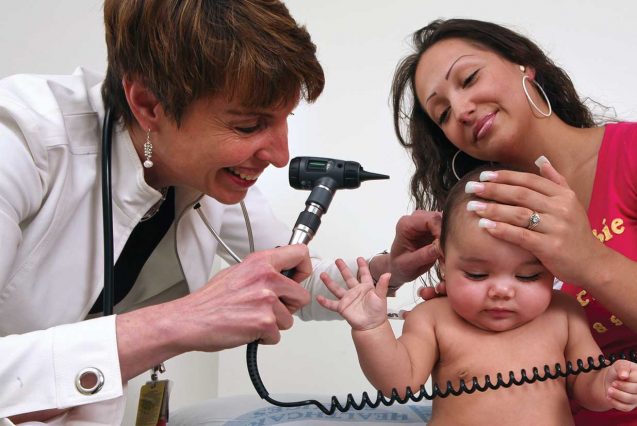
Connecting patients in need with compassionate care providers

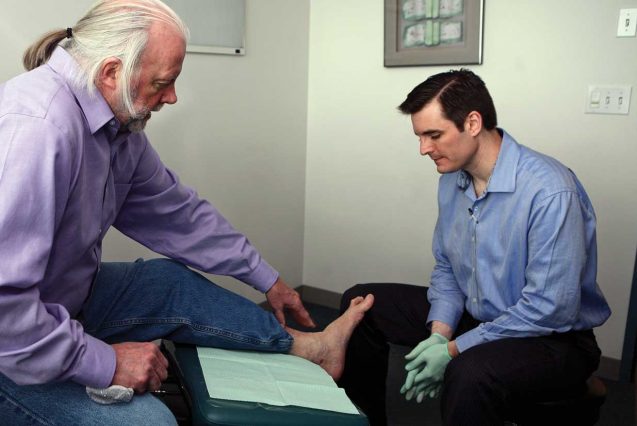
Care Coordination is at the heart of what we do. Our care coordinators help committed patients navigate a sometimes complex health care system and connect with compassionate doctors willing to provide the services they need.
What is our Care Coordination Program?
Project Access Northwest connects un- and under-insured patients with the specialty care they need.
Who is eligible for the Care Coordination Program?
Our care coordination program focuses on patients who are uninsured or enrolled with Apple Health. We are partnering with patients who have a primary care medical provider in a safety net clinic and have a specialty health care need, but no specialty provider.
How does the Care Coordination Program work?
When the care of a specialist is required, the primary care/family doctor from a community health care center or free clinic makes a referral to Project Access Northwest.
Our intake person reviews the enrollment form for completeness. Once the referral is accepted, a registered nurse reviews that referral to determine the appropriate specialty and to ensure that all needed labs, tests and diagnostic imaging are included. The care coordinator then works with the patient to schedule the first appointment. Follow-up appointments with the same provider may be scheduled directly with the provider's office.
The patient receives:
- Confirmation of specialist appointment
- Transportation details, including maps, parking instructions and public transportation options when available
The specialist receives:
- An informed and engaged patient
- All the information needed for the patient’s care at the time of the initial visit
- A patient who shows up for his/her appointments.
Our program proudly boasts a greater than 95% appointment success rate, compared to the Medicaid/uninsured average of 70 percent.
Why is the Care Coordination Program important?
Project Access Northwest removes the barriers to the client’s accessing care while reducing the paperwork and management burden on the specialty care provider. This enables providers to focus on care and serve a larger number of low-income patients.
Related Entries:
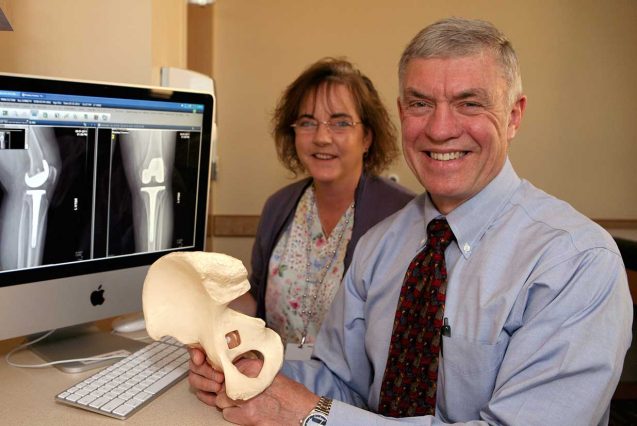
Provider Stories
Learn more about our providers who volunteer their time to care for patients in need.